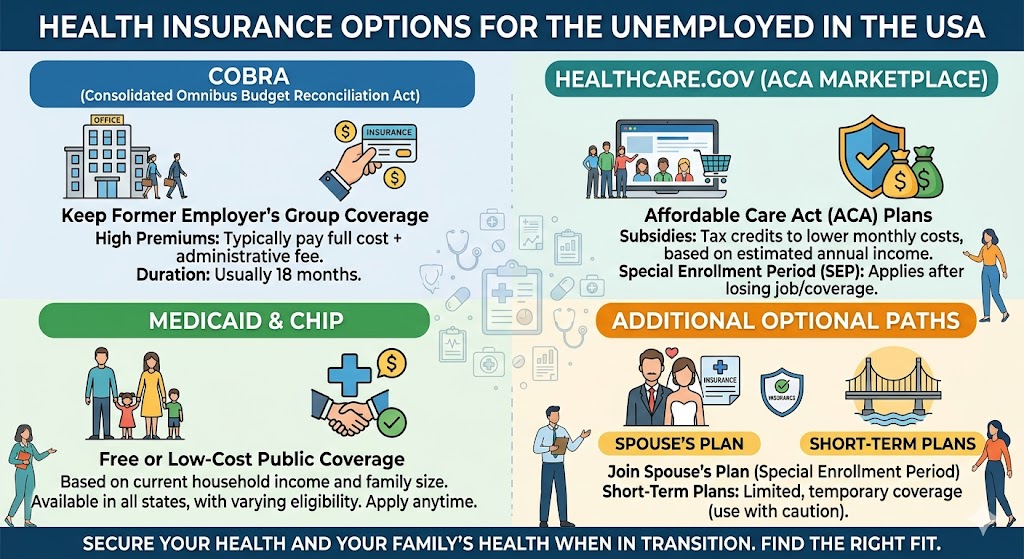
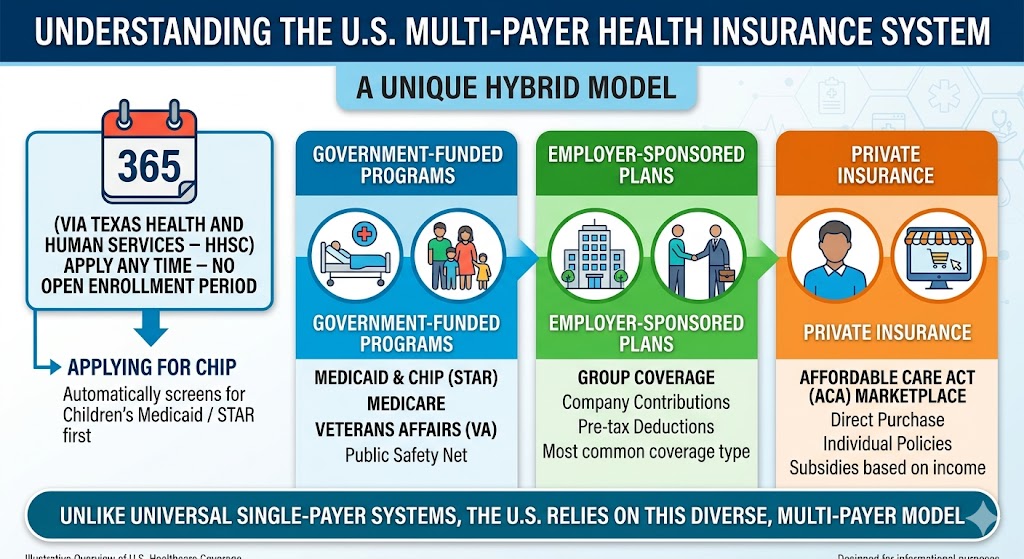
Losing your job is stressful enough without the added fear of a medical emergency wiping out your savings. In the United States, when the paycheck stops, your health coverage often stops with it—but it doesn’t have to stay that way. For the millions of Americans navigating unemployment, the path to affordable healthcare runs through three distinct federal programs: COBRA, Medicaid, and the ACA Marketplace. Each option operates under completely different eligibility rules, timelines, and cost structures.
COBRA lets you keep your former employer’s plan, but you’ll pay the full premium out of pocket—often a staggering 600to600to2,500 per month. Medicaid, by contrast, offers free or nearly free coverage but is only available if your state expanded eligibility and your household income falls below a specific threshold (typically 138% of the Federal Poverty Level).
Meanwhile, the ACA Marketplace provides subsidized private plans that can cost as little as $0 per month—but only if you enroll during a 60-day Special Enrollment Period triggered by your job loss. Understanding which door to knock on, and how quickly you need to act, is the difference between staying protected and facing bankruptcy over a broken bone.
This guide breaks down the exact eligibility criteria for all three programs in 2026, so you can secure coverage before the clock runs out.
1. COBRA (Continuation of Employer Coverage)
COBRA lets you keep your previous employer’s group health plan (medical, dental, vision) temporarily after losing job-based coverage.
Key Eligibility Criteria:
- Your employer must have had 20 or more employees in the previous year.
- You were enrolled in the employer’s group health plan right before the qualifying event.
- Qualifying event: Job loss (voluntary quit or layoff) for any reason except gross misconduct, reduction in hours, or other life events (divorce, death of covered employee, etc.).
- You generally have 60 days from the date coverage ends (or notice is provided) to elect COBRA.
Duration: Typically 18 months for job loss (can extend in some cases). Cost: You pay the full premium + 2% admin fee (often 100%+ more expensive than when employed, since employers usually subsidize part of it). Best for: People who want to keep the exact same doctors/network short-term and can afford the high cost.
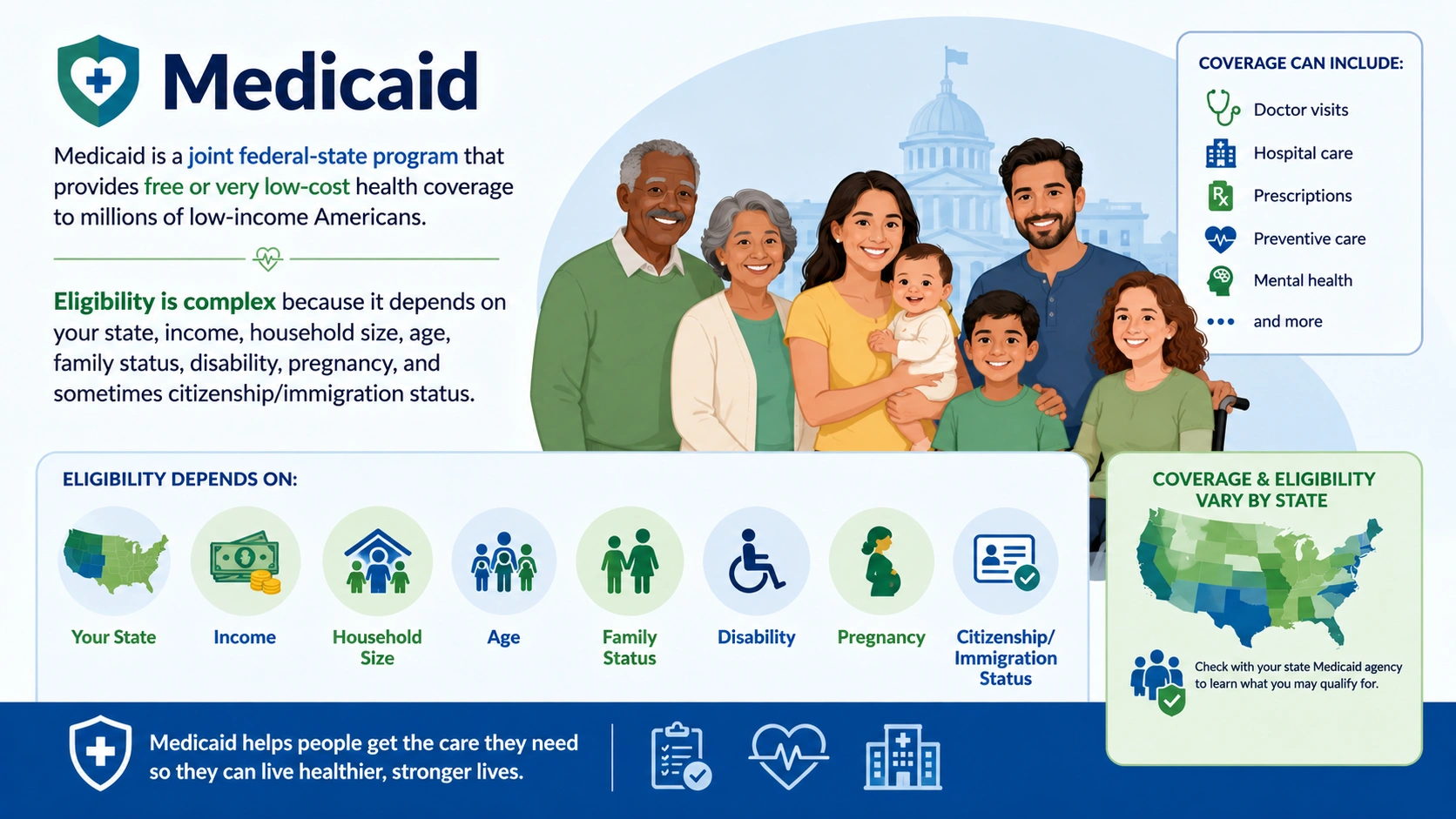
2. Medicaid (State-Federal Low-Income Program)
Medicaid provides free or very low-cost coverage. Eligibility is highly state-specific and primarily income-based.
Key Eligibility Criteria:
- U.S. citizen or eligible immigrant.
- Resident of the state where applying.
- Income usually below certain % of the Federal Poverty Level (FPL).
- In Medicaid expansion states (most states): Adults under 65 with income up to ~138% FPL (roughly $15,000–$20,000+ for a single person in 2026, depending on state and household size) often qualify regardless of having children.
- In non-expansion states: Stricter limits; many childless adults may not qualify unless pregnant, disabled, or in specific categories.
- Other factors: Household size, pregnancy, disability, or having children.
Tip: Unemployment often lowers your income enough to qualify, especially if you have little other income. Apply even if unsure — many states have simplified processes.
2026 FPL reference (approximate): ~$15,960 for one person; higher for larger households.
3. ACA Marketplace (HealthCare.gov or State Exchange)
These are private plans you buy with possible subsidies. Losing job-based coverage triggers a Special Enrollment Period.
Key Eligibility Criteria:
- Live in the U.S.
- U.S. citizen/national or lawfully present.
- Not incarcerated.
- No upper income limit to enroll, but premium subsidies (tax credits) are available mainly for household incomes 100%–400% FPL (with enhanced subsidies still helping many above that in practice).
- You must not have affordable employer coverage available (COBRA is considered but often unaffordable, so many qualify for subsidies).
Special Enrollment: You have 60 days before or after losing job coverage to enroll. Subsidies: Based on your expected annual household income. Can make plans very affordable or $0 premium for lower incomes.
Quick Comparison for Unemployed People
| Option | Best If Your Income Is… | Cost to You | How Long? | How to Apply |
|---|---|---|---|---|
| COBRA | Higher (can afford premiums) | Full premium + 2% | 18 months typical | Through former employer |
| Medicaid | Very low | Usually $0 or very low | Ongoing (if eligible) | State Medicaid agency |
| ACA Marketplace | Low to moderate | Subsidized premiums | Renewable yearly | Healthcare.gov (or state site) |
Recommendation: Start at Healthcare.gov — fill out one application and it will tell you if you qualify for Medicaid, CHIP, or subsidized Marketplace plans. You can compare options side-by-side.
Would you like me to expand on any specific state, income examples, or how to apply? Or generate another visual (e.g., eligibility flowchart or comparison infographic)?
Health insurance eligibility for unemployed people varies significantly by state, primarily due to Medicaid rules. COBRA and ACA Marketplace rules are mostly federal with some state nuances.
2026 Federal Poverty Level (FPL) Guidelines (48 Contiguous States)
- 1 person: $15,960 annual (~$1,330/month)
- 138% FPL (key for Medicaid expansion): ~$22,025 annual (~$1,835/month)
- Higher for larger households (add ~$5,680 per additional person at 100% FPL).
1. COBRA
Federal rules apply nationwide with little state variation for employers with 20+ employees:
- Up to 18 months (extensions possible to 29/36 months in some cases).
- You pay full premium + 2% admin fee.
- State mini-COBRA: Some states have rules for smaller employers (<20 employees), with varying durations (often shorter). Check your state’s Department of Insurance.
2. Medicaid (Biggest State Differences)
Expansion states (41 states + DC): Low-income adults (under 65, no dependents needed) generally qualify up to ~138% FPL based primarily on income. Unemployment often drops income enough to qualify.
Non-expansion states (roughly 10): Stricter rules. Childless adults often have very limited or no eligibility unless pregnant, disabled, or in specific categories. Parents may qualify at lower thresholds.
Non-expansion states (as of 2026): Alabama, Florida, Georgia, Kansas, Mississippi, South Carolina, Tennessee, Texas, Wisconsin (partial), Wyoming (and possibly others with limited programs).
Examples (approximate monthly income limits for adults; check exacts as they update):
- Expansion examples (138% FPL range): California, New York, Illinois, etc. — often ~$1,800+/month for a single person.
- Non-expansion examples: Texas, Florida — limited pathways; many unemployed adults fall into the “coverage gap” and rely on ACA with potential subsidies.
Other notes: Some states have work requirements or more frequent renewals. Unemployment benefits count as income, but many still qualify. Apply via your state Medicaid agency or Healthcare.gov.
3. ACA Marketplace (HealthCare.gov or State Exchange)
Federal rules with state variations in plan options, premiums, and extra subsidies:
- Special Enrollment Period (60 days) after job loss.
- Subsidies available from ~100%–400% FPL (with a “cliff” returning in 2026 as enhanced subsidies sunset). Lower incomes get more help.
- In non-expansion states, you may get better subsidies if you don’t qualify for Medicaid.
- Some states (e.g., CA, NY, MA) offer additional state subsidies.
Recommendation: Visit Healthcare.gov and enter your state + income/household details. It screens for Medicaid, CHIP, and subsidized Marketplace plans in one application. This is the fastest way to see your specific eligibility.
Would you like details for a specific state (or a few), income examples for different household sizes, or a visual comparison chart? Let me know!