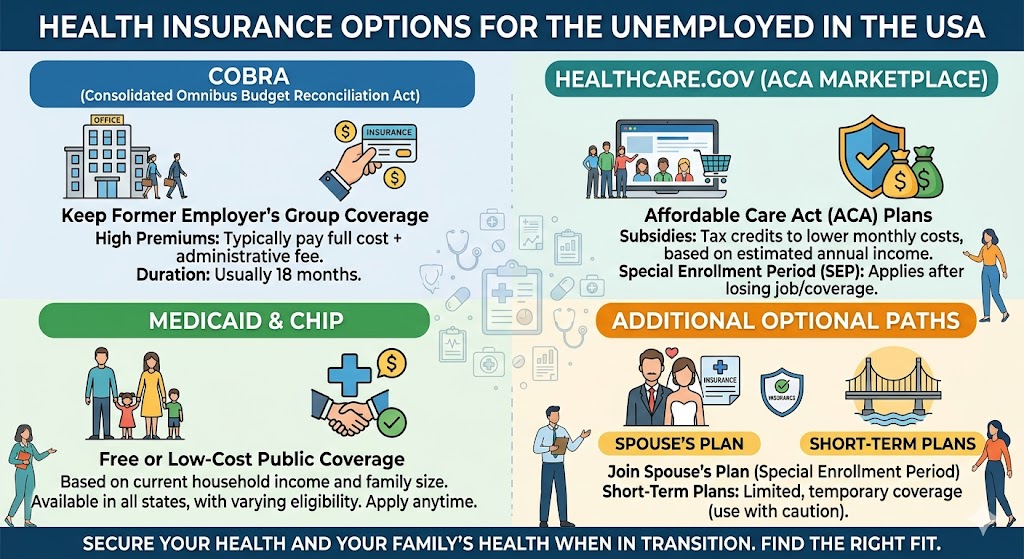
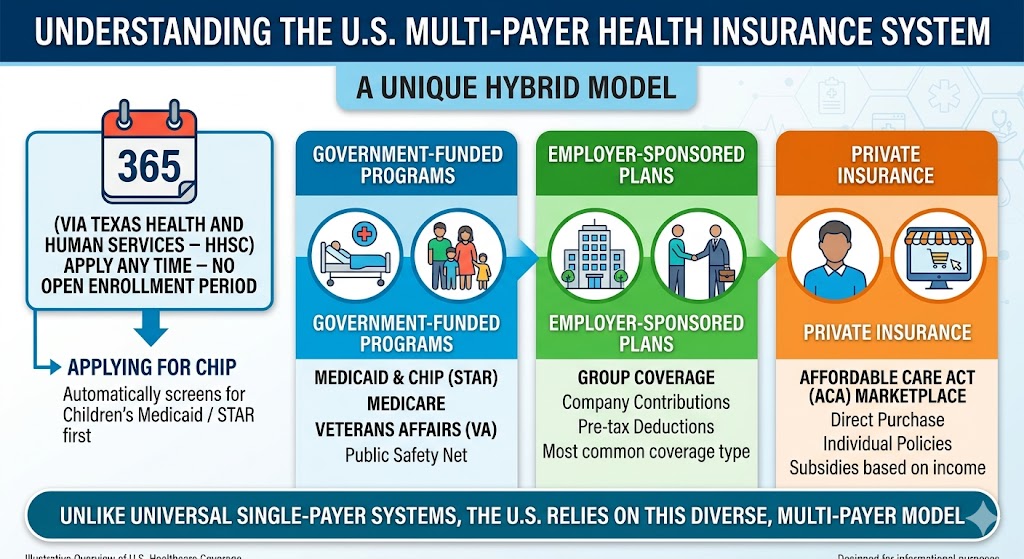
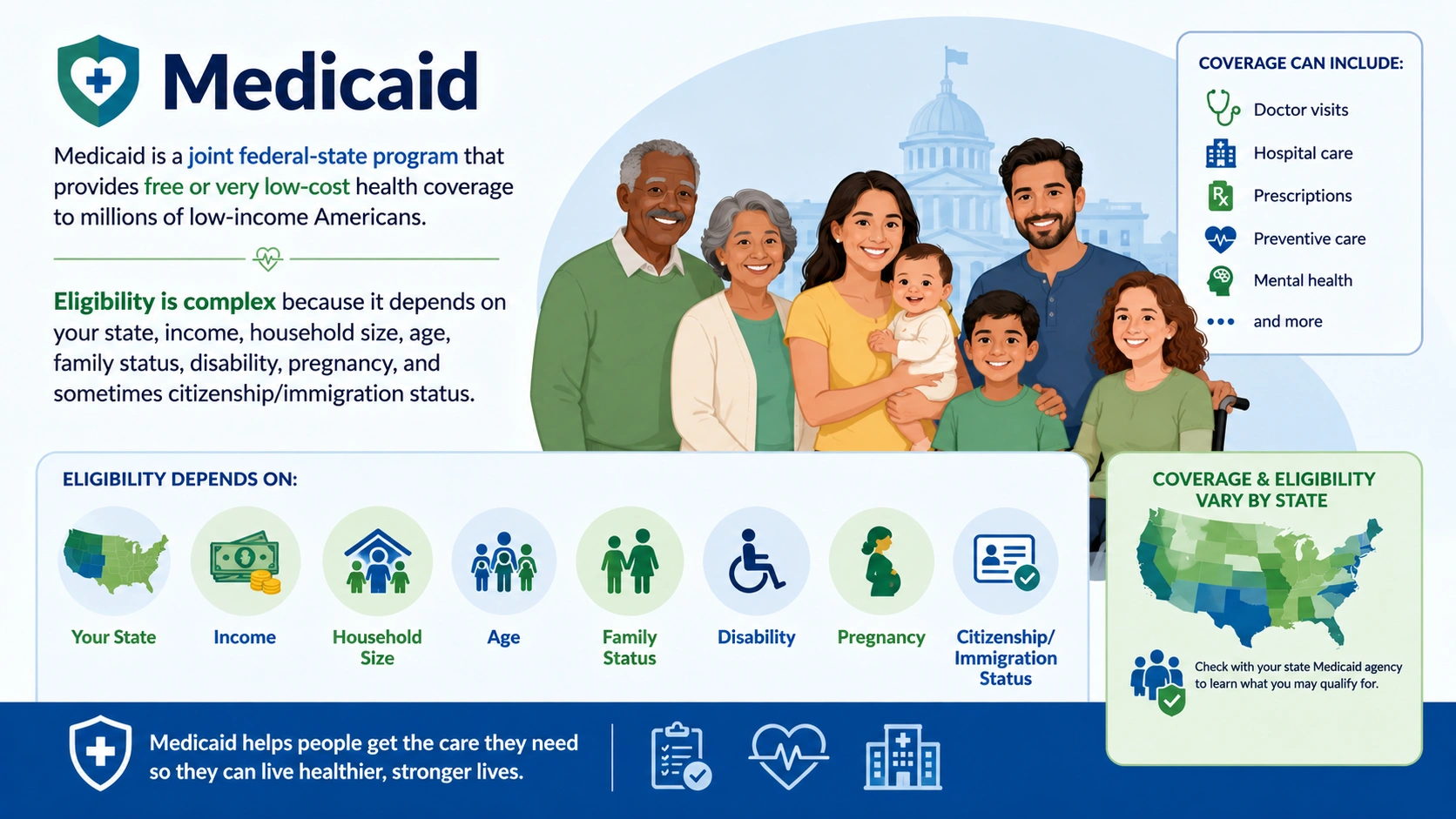
Every child deserves access to healthcare, but for millions of American families, the cost of private insurance puts it out of reach. At the same time, their income is too high to qualify for Medicaid. This is precisely the gap that the Children’s Health Insurance Program (CHIP) was designed to fill.
CHIP (Children’s Health Insurance Program) provides low-cost or free health coverage for children in families that earn too much for Medicaid but cannot afford private insurance. It is a joint federal-state program, so eligibility (especially income limits) varies significantly by state.
This comprehensive guide explains everything you need to know about CHIP: eligibility requirements, how it differs from Medicaid, what services are covered, how much it costs, how to apply, and what happens when your child turns 19. We also include state-by-state variations, income limit examples, and practical recommendations for unemployed parents who may find their children newly eligible due to reduced household income.
Table of Contents
- What Is CHIP? An Overview
- General CHIP Eligibility Criteria
- Key Point for Unemployed Parents
- 2026 Federal Poverty Level (FPL) Reference
- CHIP vs. Medicaid: Understanding the Difference
- Income Limits Overview
- State-by-State Variability
- State Variations (Selected Examples)
- Health Services Covered by CHIP
- Costs: Premiums, Copays, and Maximums
- How to Apply for CHIP
- Special Rules: Continuous Eligibility and Retroactive Coverage
- What Happens When Your Child Turns 19
- Frequently Asked Questions
- Recommendation
What Is CHIP? An Overview
The Children’s Health Insurance Program—originally called the State Children’s Health Insurance Program (SCHIP)—was established in 1997 under Title XXI of the Social Security Act. The program was created specifically to address a persistent problem in American healthcare: families who worked hard but still couldn’t afford private insurance, yet earned just enough to be disqualified from Medicaid.
CHIP provides federal matching funds to states to initiate and expand health insurance coverage to uninsured, low-income children. The program is funded jointly by the federal government and the states, with the federal government contributing a higher match rate than it does for Medicaid. As of 2026, CHIP is funded through fiscal year 2027.
Key Features of CHIP:
- Covers children up to age 19 (though age limits vary slightly by state)
- Available to families with incomes too high for Medicaid
- Costs never exceed 5% of a family’s annual income
- Coverage includes medical, dental, and vision care
- Application is free and can be done at any time (no enrollment window restrictions)
General CHIP Eligibility Criteria
Children typically qualify for CHIP if they meet these requirements:
| Criterion | Detail |
|---|---|
| Age | Under 19 years old (some states cover up to age 20 or 21 in certain cases) |
| Immigration/Citizenship | U.S. citizen, national, or lawfully present immigrant |
| Residency | Resident of the state |
| Insurance Status | Uninsured (not covered by other creditable coverage like employer plans; there may be a waiting period in some states) |
| Income | Family income above the state’s Medicaid limit but within the state’s CHIP income threshold (usually based on Modified Adjusted Gross Income — MAGI) |
| Other factors | Not incarcerated; may have additional state-specific rules |
Important Note on Insurance Status: Some states impose a “waiting period” before a child can enroll in CHIP if they had other creditable coverage (like an employer plan) that was voluntarily dropped. This is designed to prevent families from dropping private insurance specifically to enroll in CHIP. However, if coverage was lost due to job loss or unaffordability, the waiting period is often waived.
Income Measurement: CHIP uses Modified Adjusted Gross Income (MAGI) to determine eligibility. MAGI includes wages, salaries, tips, unemployment compensation, and certain other income sources. It is the same income calculation method used for ACA Marketplace subsidies, creating consistency across programs.
Key Point for Unemployed Parents
Unemployment often reduces household income, making children more likely to qualify for Medicaid (free) or CHIP (low-cost).
If you have recently lost your job or experienced a reduction in work hours, your household income has likely dropped significantly. This change in circumstances can push your family from being ineligible for assistance to being fully qualified for either Medicaid or CHIP.
The One-Application Advantage: You do not need to figure out which program you qualify for on your own. Apply even if unsure — one application usually screens for both Medicaid and CHIP. When you submit a single application through Healthcare.gov or your state’s agency, the system automatically evaluates your child’s eligibility for Medicaid first. If they don’t qualify for Medicaid (because your income is above that threshold), the system then checks CHIP eligibility. If they don’t qualify for CHIP, it may direct you to subsidized ACA Marketplace plans.
Action Step for Unemployed Parents: Do not wait. As soon as your income decreases due to job loss or reduced hours, submit a CHIP/Medicaid application. You may qualify for retroactive coverage that pays for medical bills incurred in the three months before your application date.
2026 Federal Poverty Level (FPL) Reference
The Federal Poverty Level (FPL) is the baseline metric used to determine eligibility for Medicaid, CHIP, and ACA subsidies. FPL numbers are updated annually by the Department of Health and Human Services.
2026 FPL Guidelines for the Contiguous United States (48 states + DC):
| Household Size | Annual Income (100% FPL) |
|---|---|
| 1 person | $15,960 |
| 2 people | $21,640 |
| 3 people | $27,320 |
| 4 people | $33,000 |
| 5 people | $38,680 |
| 6 people | $44,360 |
| Each additional person | Add approximately $5,680 |
Special Note for Alaska and Hawaii: Both states have higher FPL guidelines due to higher costs of living. Alaska’s FPL for a family of 4 is approximately 41,250(2026estimate),andHawaii′sisapproximately41,250(2026estimate),andHawaii′sisapproximately37,950. Always use your state’s specific FPL numbers when applying.
How to Use FPL Percentages: If a state offers CHIP up to 250% FPL, multiply the 100% FPL number for your family size by 2.5. For a family of 4 (100% FPL = 33,000),25033,000),25033,000 × 2.5 = $82,500 annual income.
How FPL Percentages Work in Practice:
| FPL Percentage | Family of 3 (100% = $27,320) | Family of 4 (100% = $33,000) |
|---|---|---|
| 138% (Medicaid expansion typical) | $37,702 | $45,540 |
| 200% | $54,640 | $66,000 |
| 250% | $68,300 | $82,500 |
| 300% | $81,960 | $99,000 |
| 400% (ACA subsidy limit) | $109,280 | $132,000 |
CHIP vs. Medicaid: Understanding the Difference
Many families confuse CHIP with Medicaid because the two programs often work together and are administered by the same state agencies. However, they serve different populations.
| Feature | Medicaid | CHIP |
|---|---|---|
| Target Population | Very low-income families, individuals with disabilities, elderly | Working families with moderate income |
| Income Eligibility | Lower threshold (typically up to 138-200%+ FPL depending on state) | Higher threshold (often 200-300%+ FPL) |
| Cost to Family | Usually $0 or very low copays | Low monthly premiums (often 0−0−50 per family, capped at 5% of income) and copays |
| Coverage | Comprehensive mandatory and optional benefits | Comprehensive benefits, but states have more flexibility |
The Coverage Continuum: In most states, there is a smooth continuum of coverage:
- Medicaid (free): Lowest income families
- Premium-free CHIP: Moderate income families who don’t qualify for Medicaid
- CHIP with premiums: Higher income families still needing assistance
In many states, children can qualify for Medicaid at lower incomes (often up to 138–200%+ FPL) and then CHIP for the next tier. Exact cutoffs depend on household size and state rules.
In practice, most states use a “one-door” application process where families apply for both programs simultaneously. The state determines whether the child qualifies for Medicaid (free coverage) or CHIP (which may have premiums) based on household income.
Income Limits Overview
CHIP income limits vary dramatically across states, ranging from about 170% to 400% FPL. Most states fall in the 200–300%+ FPL range.
General Rule: Many states set higher income limits for children than for adults. This reflects the policy priority of covering children even when parents may not qualify for assistance.
Approximate Annual Income for a Family of 4 at Upper CHIP Limit:
| CHIP Limit (FPL) | Annual Income (Family of 4) |
|---|---|
| ~200–210% FPL (lower-limit states) | 66,000–66,000–69,000 |
| 250–300% FPL (mid-range states) | 82,500–82,500–99,000 |
| 400% FPL (higher states, e.g., NY) | Over $132,000 |
Important Note on the 5% Disregard: Many states apply a 5% income disregard when calculating eligibility. This means that a small amount of income (up to 5% of the FPL) is subtracted from your gross income before comparing to the limit. In practice, this slightly raises the effective income cutoff. For example, a state with a 200% FPL limit plus a 5% disregard effectively allows income up to 205% FPL. The examples in this guide reflect pre-disregard numbers; actual allowable income in your state may be slightly higher.
State-by-State Variability: Why Location Matters
Because CHIP is a joint federal-state program, eligibility rules, benefits, and costs differ significantly depending on where you live. This section highlights key areas of variability.
Income Thresholds
States set their own CHIP income limits. Some states cap CHIP eligibility at 200% FPL, while others extend coverage to families earning 300% FPL or more.
Premium Structures
States have considerable flexibility in designing premium requirements. The general federal rule is that total premiums and cost-sharing cannot exceed 5% of a family’s annual income. However, states decide:
- At what income level premiums begin (often around 150-200% FPL)
- Whether premiums are charged per child or per family
- Whether premium payments are monthly, quarterly, or annual
Coverage Extensions
Some states have used federal waivers to extend CHIP coverage to populations beyond children, including pregnant women and parents. As of 2026:
- 7 states use CHIP funding to cover pregnant individuals
- 25 states provide coverage from conception to birth (FCEP option)
Managed Care Organizations (MCOs)
States contract with private insurance companies—called Managed Care Organizations—to deliver CHIP benefits. The number and type of MCOs available vary by state.
How to Find Your State’s Rules
The official USAGov website provides a state-by-state CHIP directory. You can also contact your state’s Medicaid/CHIP agency directly.
State Variations (Selected Examples)
To illustrate how CHIP income limits vary across the country, here are selected examples from recent data. These numbers are approximate and subject to change; always verify with your state’s official CHIP agency.
| State | CHIP Income Limit (FPL) | Approx. Annual Limit for Family of 4 | Notes |
|---|---|---|---|
| California | Up to 266% FPL via Medi-Cal; higher via county programs | ~$87,800 | Some counties offer expanded coverage beyond standard CHIP limits |
| New York | Up to 400% FPL | ~$132,000+ | One of the highest CHIP limits in the nation |
| Texas | Approximately 200%+ FPL (after Medicaid threshold) | ~$66,000+ | Texas has not expanded Medicaid, but CHIP remains available |
| Florida | Approximately 210% FPL | ~$69,300 | |
| North Carolina | Approximately 210% FPL | ~$69,300 | |
| Illinois | 300%+ FPL | ~$99,000+ | |
| Pennsylvania | 300%+ FPL | ~$99,000+ | No family makes too much for CHIP in PA; higher incomes pay higher premiums |
Important Clarification: In many states, children can qualify for Medicaid at lower incomes (often up to 138–200%+ FPL depending on the state). CHIP then covers the next income tier above the Medicaid threshold up to the state’s maximum CHIP limit. For example, in Texas, children might qualify for Medicaid up to approximately 150-175% FPL, then CHIP from that point up to roughly 200% FPL. The exact crossover point varies by family size and state rules.
Example Scenario – California: A family of four in California earning 80,000peryear(approximately24280,000peryear(approximately24295,000 (approximately 288% FPL) might still qualify for CHIP through county-specific programs or premium assistance.
Example Scenario – New York: A family of four earning $130,000 per year (approximately 394% FPL) would qualify for CHIP. This makes New York one of the most generous states for child health coverage.
Health Services Covered by CHIP
While states have flexibility in designing their CHIP programs, all CHIP plans must cover a comprehensive set of health services. According to the CDC and state CHIP programs, covered services include:
Medical Services:
- Routine checkups and well-child visits
- Doctor visits (primary care and specialists)
- Immunizations (vaccines)
- Hospital care (inpatient and outpatient)
- Emergency services
- Surgery
- Laboratory and X-ray services
- Prescription medications
Behavioral Health:
- Mental health services
- Substance use disorder treatment
Vision Services:
- Eye exams
- Glasses and contact lenses
Dental Services:
- Dental exams and cleanings
- X-rays
- Fillings
- Extractions
- Root canals
- Crowns
- Medically necessary orthodontics (in many states)
Some states offer additional benefits beyond the federal minimum requirements, so checking your state’s specific CHIP coverage details is recommended.
Costs: Premiums, Copays, and Maximums
CHIP is designed to be affordable for working families. While coverage is not always free, costs are strictly limited.
The 5% Rule
Total annual family spending on CHIP premiums and cost-sharing (copays, deductibles) cannot exceed 5% of the family’s annual income. This is a hard federal cap that protects families from unaffordable healthcare costs.
Premiums
Premiums vary based on income and family size. General patterns:
| Income Level | Typical Premium Structure |
|---|---|
| Lower income (e.g., up to 150-200% FPL) | $0 (premium-free CHIP) |
| Moderate income (e.g., 200-250% FPL) | Low monthly premiums (10−10−20 per child, often with family maximums) |
| Higher income (e.g., 250-300%+ FPL) | Higher but still capped premiums (often 20−20−50 per child, with family maximums) |
Many states offer premium-free CHIP at lower income levels within the CHIP range. For example, a family might get free CHIP up to 200% FPL, then pay modest premiums for income between 200% and 300% FPL.
Copays and Cost-Sharing
States may charge small copays for certain services, such as:
- Doctor visits (5−5−15)
- Prescription medications (3−3−8 for generics; slightly more for brand-name)
- Non-emergency use of the emergency room (higher copay — often 25−25−50 — to discourage inappropriate ER use)
Preventive services (well-child visits, immunizations) are covered with no cost-sharing in all CHIP programs.
States are required to track family-based cost-sharing and waive cost-sharing once a family reaches the 5% maximum.
Medicaid vs. CHIP Costs Summary
| Program | Typical Premiums | Typical Copays |
|---|---|---|
| Medicaid | Usually $0 | 0orverylow(often0orverylow(often0 for children) |
| CHIP | Often 0–0–50 per family | Low (e.g., 5doctorvisit,5doctorvisit,3 prescription) |
| Cap | Total family spending cannot exceed 5% of annual income |
How to Check & Apply
One of the best features of CHIP is that you can apply at any time—there is no annual open enrollment period. You can apply in several ways:
Option 1: Visit Healthcare.gov (Recommended)
Create an account at Healthcare.gov (or your state’s Marketplace/insurance site) and fill out one application — it screens for Medicaid, CHIP, and ACA subsidies simultaneously.
- If you qualify for Medicaid or CHIP, the system will forward your information to your state agency.
- If you do not qualify, you will see subsidized ACA Marketplace plans.
- This is the most efficient method because one application checks all three programs.
Option 2: Go Directly to Your State’s CHIP Agency
Search online for “[your state] CHIP” or “[your state] Medicaid” to find your state’s direct application portal.
- Examples: Texas CHIP, Florida KidCare, New York Child Health Plus
- Many states allow online, phone, mail, or in-person applications
Option 3: Apply by Phone or Mail
Call your state’s CHIP hotline (available 24/7 in many states). Request a paper application if you prefer.
Information You Will Need
Before you apply, gather:
- Employer and income information (pay stubs, W-2 forms, unemployment benefit statements)
- Social Security numbers for all household members applying
- Dates of birth
- Immigration documentation (if applicable)
- Policy numbers for any current health insurance
Tips for a Smooth Application
- Submit one application for all children under 19 living in the same household
- Answer all questions completely — incomplete applications delay processing
- Include unemployment benefits as income if you are receiving them
- If your income has recently changed (due to job loss), report your current income, not last year’s
After Approval
Once your application is approved, you will:
- Receive a welcome packet and member ID card in the mail
- Be asked to select a Managed Care Organization (health plan) if your state offers choices
- Have coverage effective from the date of approval (or potentially retroactively)
Special Rules: Continuous Eligibility and Retroactive Coverage
Federal law provides important protections for children enrolled in CHIP to prevent gaps in coverage.
12-Month Continuous Eligibility
As of January 1, 2024, states must provide 12 months of continuous coverage for children ages 18 and under in both CHIP and Medicaid. This means that once a child is enrolled, they remain covered for a full year even if the family’s income changes slightly. This eliminates the “churn” of moving on and off coverage due to minor income fluctuations.
Presumptive Eligibility
Some states offer “presumptive eligibility,” which allows certain qualified entities—such as schools, hospitals, and community health centers—to screen for CHIP and Medicaid eligibility and immediately enroll eligible children without waiting for the full application to be processed. This ensures that children get coverage right away when they need care.
Retroactive Coverage
Medicaid and CHIP programs may offer retroactive coverage for the three months before the application date. If your child received medical care in the 90 days before you applied, those bills might be covered. You must request retroactive coverage when applying. This is particularly valuable for families who delayed applying due to job loss or other disruptions.
What Happens When Your Child Turns 19
CHIP coverage generally ends when a child reaches age 19. Some states cover up to age 20 or 21, but most follow the federal baseline of under 19.
Options After CHIP Ends
When your child ages out of CHIP, they have several options:
- Medicaid: If they have a disability or very low income, they may qualify for adult Medicaid.
- ACA Marketplace Plan: Young adults can purchase their own health insurance through Healthcare.gov. Depending on their income, they may qualify for premium tax credits that lower monthly costs.
- Parent’s Plan (until age 26): Under the ACA, young adults can remain on a parent’s employer or Marketplace plan until age 26. If the parent has coverage, this is often the simplest option.
- Employer Coverage: If the young adult has a job that offers health insurance, they can enroll during their employer’s open enrollment or within 60 days of a qualifying life event (such as aging out of CHIP).
- Student Health Plans: Many colleges and universities offer affordable student health insurance plans for enrolled students.
Frequently Asked Questions
Q1: Can undocumented immigrant children get CHIP?
In some states, yes. As of 2026, 25 states provide coverage from conception to birth through the FCEP option regardless of the pregnant person’s immigration status. For older children, rules vary by state. Some states have used federal waivers to extend CHIP coverage to all children regardless of immigration status, while others have not. Lawfully present immigrants are eligible in all states.
Q2: How long does it take to get approved for CHIP?
Processing times vary by state, but approval typically takes 30 to 45 days from the date of application. If you are approved, coverage may be retroactive for up to three months before your application date.
Q3: Can adults get CHIP?
Generally, no. CHIP is primarily for children under 19. However, some states have received federal permission to extend CHIP coverage to pregnant women (7 states) and, in rare cases, parents.
Q4: Do I have to wait for open enrollment to apply for CHIP?
No. Unlike ACA Marketplace plans, CHIP has no open enrollment period. You can apply at any time of the year.
Q5: What if I’m denied CHIP coverage?
If you are denied because your income is too high, your child may still qualify for subsidized coverage through the ACA Marketplace. If you are denied for other reasons (e.g., residency or citizenship issues), you can appeal the decision through your state’s appeals process.
Q6: Does CHIP cover dental and vision?
Yes. All CHIP programs must cover dental and vision services. Dental coverage typically includes exams, cleanings, x-rays, fillings, and in some states, orthodontics.
Q7: How is CHIP funded in 2026?
CHIP is currently funded through fiscal year 2027. The Bipartisan Budget Act of 2018 extended CHIP funding, and the program remains operational with federal matching funds available to states.
Q8: Do I need to report income changes?
Yes. While children get 12 months of continuous coverage once enrolled, you should report significant income changes to your state agency. If your income increases substantially, you may be moved from premium-free CHIP to CHIP with premiums, or you may be required to transition to a Marketplace plan at the next renewal. If your income decreases, your child may become eligible for Medicaid (even lower costs).
Q9: What is the difference between MAGI and gross income?
MAGI (Modified Adjusted Gross Income) is the specific income calculation method used for CHIP, Medicaid, and ACA subsidies. It includes wages, salaries, tips, unemployment compensation, Social Security benefits, and certain other income. It generally excludes non-taxable income like child support. Most states use MAGI for CHIP eligibility.
Q10: Can I have CHIP and private insurance at the same time?
Generally, no. CHIP is for uninsured children. If you have access to affordable employer coverage, your child will not qualify for CHIP. However, if the employer coverage is unaffordable (costing more than a certain percentage of income), some states may allow CHIP as secondary coverage or provide premium assistance to help you pay for the employer plan.
Recommendation
Navigating CHIP eligibility can feel overwhelming because of the state-by-state variations in income limits, premiums, and rules. However, the process itself is simple:
Use the official tools with your exact household size, income (including unemployment benefits), and state for a personalized determination.
Step-by-Step Recommendation:
- Do not guess. Income limits vary too much by state for general rules to be reliable for your specific situation.
- Apply online at Healthcare.gov or your state’s Marketplace. One application takes about 30 minutes and screens for Medicaid, CHIP, and ACA subsidies.
- Include all income. Report wages, unemployment benefits, child support, and any other income accurately.
- Apply even if unsure. Many families assume they earn too much and never apply. You may be surprised by your state’s CHIP limits—especially if your income has dropped due to unemployment.
- If your income fluctuates, apply when it is lowest. You can always report changes later.
- For unemployed parents specifically: Job loss is a qualifying life event that reduces household income. Apply as soon as your income drops. Your children may now qualify for free Medicaid or low-cost CHIP even if they didn’t qualify before.
Would you like details for a specific state, examples for different family sizes, a comparison table, or another visual (e.g., CHIP eligibility flowchart)? Let me know!
Summary: Key Takeaways
| Question | Answer |
|---|---|
| What is CHIP? | Low-cost or free health coverage for children in families who earn too much for Medicaid but can’t afford private insurance |
| Who does CHIP cover? | Children under 19 (some states up to 20-21) who are uninsured, state residents, and lawfully present |
| What are the income limits? | Range from ~170% to 400% FPL depending on state (most commonly 200–300%+) |
| Example for family of 4 | Lower-limit states: ~66,000–66,000–69,000; Mid-range: ~82,500–82,500–99,000; Higher (NY): over $132,000 |
| When can I apply? | Any time — no open enrollment period required for CHIP/Medicaid |
| How much does it cost? | Often $0 at lower income levels within CHIP range; premiums capped at 5% of income |
| What services are covered? | Medical, dental, vision, prescriptions, mental health, emergency care |
| What happens at age 19? | CHIP ends; options include parent’s plan (until 26), Marketplace, employer, or student plans |
| How do I apply? | Healthcare.gov or your state’s CHIP agency — one application screens for all programs |
Final Thoughts
CHIP represents one of the most successful public-private partnerships in American healthcare. Since its creation in 1997, the program has dramatically reduced the number of uninsured children in the United States—from nearly 15% in the late 1990s to under 5% today.
If you are a parent or guardian who works hard but struggles to afford private insurance—especially if you have recently become unemployed and your household income has dropped—apply for CHIP. The application is free, the coverage is comprehensive, and the cost is limited by law to a percentage of what you earn. Because eligibility rules vary by state, you may qualify even if you think your income is too high.
Next Steps:
- Visit Healthcare.gov or your state’s CHIP website
- Gather your income and household information (including unemployment benefits if applicable)
- Submit one application (it takes about 30 minutes)
- Select a health plan if your state offers choices
- Get your child the coverage they deserve
No child should go without healthcare because of cost. CHIP ensures that working families have a safety net—and it starts with a simple application.