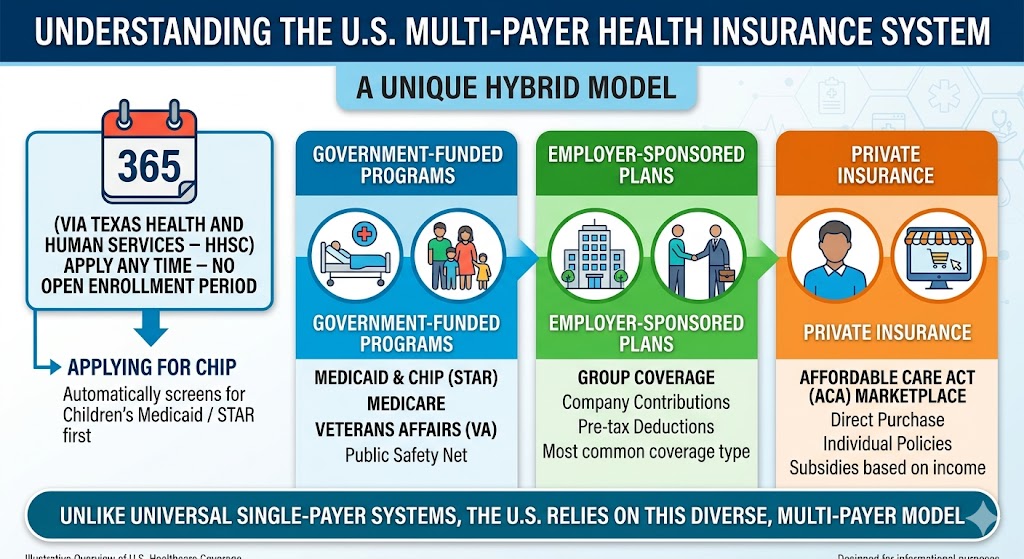
(via Texas Health and Human Services – HHSC) You can apply for CHIP (and it will automatically screen for Children’s Medicaid / STAR first) at any time — there is no open enrollment period.
Health insurance coverage in the United States operates as a unique hybrid system, blending private insurance, employer-sponsored plans, and government-funded programs. Unlike most other developed nations that have universal single-payer systems, the U.S. relies on a multi-payer model where coverage is not guaranteed by the government but is instead accessed through various pathways.
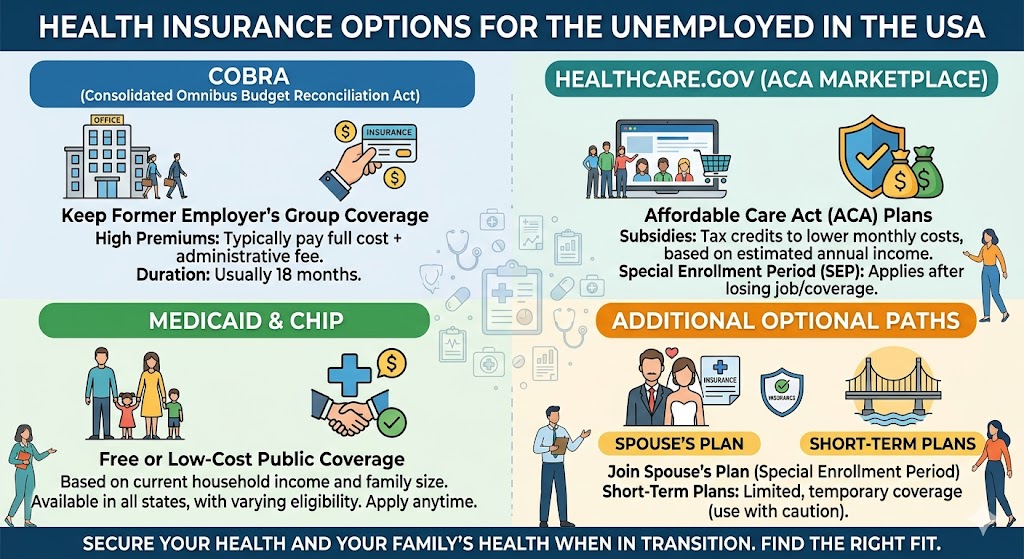
As of 2026, approximately 92% of Americans have some form of health insurance, yet roughly 26 million remain uninsured. The primary routes to coverage include employer-sponsored insurance (the most common, covering about 49% of the non-elderly population), individually purchased plans (including ACA Marketplace plans), and public programs like Medicare (for seniors 65+ and certain disabled individuals), Medicaid (for low-income individuals and families), and CHIP (for children in working families).
The Affordable Care Act (ACA), enacted in 2010, fundamentally reshaped the landscape by establishing federal subsidies, prohibiting denial of coverage for pre-existing conditions, and creating state-based Marketplaces where individuals can compare and purchase plans.
The private insurance market dominates the American system. For employed individuals, the employer typically shoulders a significant portion of the monthly premium—often 70% to 85% for employee-only coverage—while the employee pays the remainder through pre-tax payroll deductions.
These plans vary widely in cost and coverage, with common structures including Health Maintenance Organizations (HMOs) that restrict care to in-network providers, Preferred Provider Organizations (PPOs) that offer greater flexibility at higher cost, and High Deductible Health Plans (HDHPs) paired with tax-advantaged Health Savings Accounts (HSAs). In 2026, the average annual premium for employer-sponsored family coverage surpassed 24,000,withemployeescontributingroughly24,000,withemployeescontributingroughly6,000 of that amount. For those without access to employer coverage—including self-employed individuals, gig workers, part-time employees, and the unemployed—the ACA Marketplace serves as the primary private option.
These Marketplace plans are categorized into four metal tiers (Bronze, Silver, Gold, and Platinum) based on actuarial value, meaning the percentage of covered medical expenses the plan pays on average. Bronze plans cover about 60% of costs (low premiums, high deductibles), while Platinum plans cover about 90% (high premiums, low deductibles).
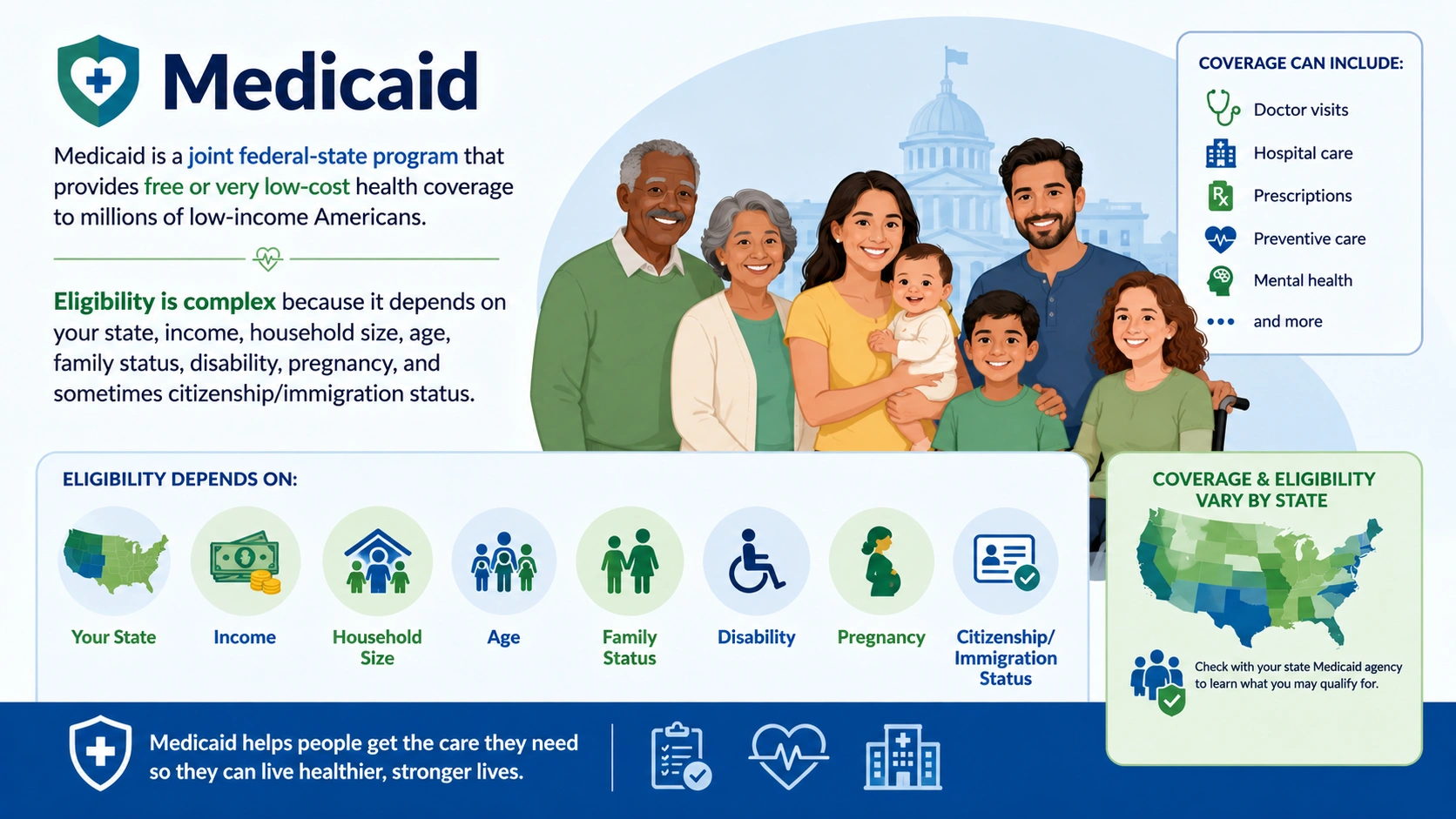
Government programs fill critical gaps for populations that private insurance does not adequately serve. Medicare, the federal program for Americans aged 65 and older, covers over 65 million people. It consists of Part A (hospital insurance, generally premium-free), Part B (medical insurance, with a standard premium of approximately $174.70/month in 2026), Part C (Medicare Advantage, private plans that bundle Parts A and B), and Part D (prescription drug coverage). Medicaid, jointly funded by federal and state governments, provides free or low-cost coverage to low-income individuals, families with children, pregnant women, elderly adults, and people with disabilities.
However, due to the Supreme Court’s 2012 ruling that made Medicaid expansion optional for states, 10 states (including Texas, Florida, and Georgia) have not expanded their programs, creating a coverage gap where adults earn too much for Medicaid but too little for Marketplace subsidies. CHIP (Children’s Health Insurance Program) specifically targets children in families that earn too much for Medicaid but cannot afford private insurance, covering over 10 million children nationwide with income limits ranging from 170% to 400% of the Federal Poverty Level depending on the state.
Despite these options, significant gaps and challenges persist. The most common barrier remains affordability, even with subsidies. Approximately 40% of uninsured adults cite cost as the primary reason for lacking coverage. High deductibles—often 3,000to3,000to8,000 for individual Marketplace plans—mean that even insured individuals may delay or forego necessary care due to out-of-pocket expenses. Additionally, provider network adequacy remains a problem, particularly in rural areas where limited competition allows dominant hospital systems to charge higher rates, which insurers pass on to consumers.
Medical debt is uniquely American; even among insured individuals, about one in five report struggling to pay medical bills, with surprise billing (though partially addressed by the No Surprises Act of 2022) still occurring in ground ambulances and certain non-emergency scenarios. The system also creates complexity in enrollment: unlike countries with automatic or universal enrollment, Americans must actively navigate open enrollment periods, special enrollment windows triggered by life events (job loss, marriage, birth of a child), and overlapping eligibility rules for Medicaid, CHIP, and subsidized Marketplace plans.
Looking toward the future, several trends are reshaping the American health insurance landscape in 2026. The expiration of pandemic-era enhanced subsidies (which ended December 31, 2025) has increased premiums for many Marketplace enrollees by 10-20%, though standard premium tax credits remain available for those with incomes between 100% and 400% FPL. States that have not expanded Medicaid face renewed legislative pressure, with ballot initiatives and state-level reforms gaining traction. Telehealth coverage, which exploded during the pandemic, has largely stabilized with most insurers covering virtual visits at parity with in-person care.
And prescription drug pricing reforms under the Inflation Reduction Act continue to phase in, allowing Medicare to negotiate prices for ten high-cost drugs, a change expected to lower premiums for Part D plans. For the average American, the most important takeaway is this: you likely qualify for some form of assistance, whether through an employer, the Marketplace (where 9 out of 10 enrollees receive subsidies), Medicaid, or CHIP. The complexity of the system should not deter you from applying; the official gateway at Healthcare.gov provides a single application that screens for all programs and determines your eligibility in under an hour.
Step-by-Step Application Process
- Gather Required Information & Documents
- Social Security numbers for the children applying.
- Proof of income (last 30 days): Paycheck stubs, unemployment benefits, tax returns, W-2s, self-employment records, etc.
- Proof of Texas residency (utility bill, lease, mail with address).
- Proof of citizenship or qualified immigration status for the child (U.S. birth certificate, passport, etc.). Parents do not need to provide their own immigration status for the child to qualify.
- Information about household size and other income/expenses (childcare, alimony, etc.).
- Submit the Application (choose one method)
- Online (Recommended): Go to YourTexasBenefits.com → “Apply for new benefits.” You can save and return to the application anytime. There’s also a mobile app.
- By Phone: Call 2-1-1 (TTY 711). Choose language, then option 2. A representative helps start the application and mails you forms to complete.
- Paper Form: Download or request a form from YourTexasBenefits.com and mail/fax it.
- In Person: Visit a local HHSC benefits office (find locations via 2-1-1 or the website) or a community partner.
- Processing Time
- HHSC usually decides within 45 business days for CHIP/Medicaid applications.
- Faster for pregnancy-related coverage (often 15 business days).
- You may receive requests for additional documents — respond quickly to avoid delays.
- After Approval
- You’ll receive an enrollment packet in the mail.
- Choose a health plan (e.g., Texas Children’s Health Plan, Superior, Community Health Choice, etc.) available in your service area.
- Select a primary care provider (doctor).
- Pay any required enrollment fee (usually $0–$50 per family per year, income-based).
- Coverage typically starts the first day of the month after approval.
Helpful Tips
- One application screens for Children’s Medicaid (free) first, then CHIP (low-cost) if income is higher.
- Unemployment benefits count as income, but job loss often helps qualification.
- You can report changes (income, address, household) anytime via YourTexasBenefits.com or the app.
- Renewals are required periodically — watch for notices.
- Free help is available from community partners, navigators, or by calling 2-1-1.
Best Starting Point: Visit YourTexasBenefits.com and start the application or use the pre-screener tool.
Would you like a list of required documents in more detail, help with a specific family size example, or information on choosing a health plan after approval?